My Mundane Professional Association Meeting is a Luxury Most Midwives Can Only Imagine
May 5, 2017 | 3 Minute ReadOn International Day of the Midwife, Emma Clark explains the importance of a privilege that is often taken for granted.
After work, once every couple of months, I have the luxury of making my way across town to the American College of Nurse-Midwives (ACNM) Washington, D.C. Affiliate meeting to spend a couple of hours eating lukewarm Peruvian chicken and discussing issues affecting midwives at the local and national level. It’s not the meetings themselves that are luxurious: they are long; there’s always too much to discuss and do and not enough time; and they’re filled with tired, occasionally grumpy midwives coming from long days in a clinic or headed into an overnight shift at a hospital. The luxury comes from the voice these meetings give us, a luxury unknown to most of the midwives around the world.
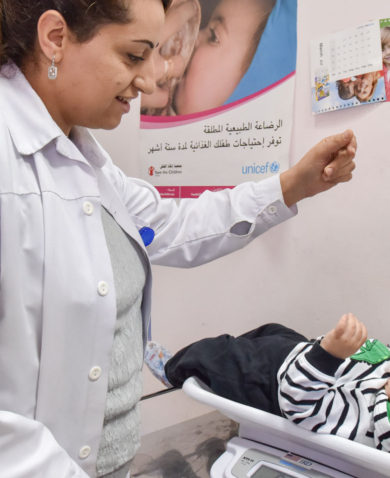
Let’s back up. Today is International Day of the Midwife, a day meant to highlight the work of midwives around the world. Officially, midwives are “skilled, knowledgeable, and compassionate” health-care providers who “care for childbearing women, newborn infants, and families across the continuum from pre-pregnancy, pregnancy, birth, postpartum, and the early weeks of life.” Because of their global presence and skills, midwives are the workhorses of maternal and newborn health (MNH) around the world. They can make or break everything from an individual childbirth experience to global targets for reductions in maternal and newborn mortality. Global efforts to reduce maternal and neonatal deaths, such as USAID’s Ending Preventable Child and Maternal Deaths and the global Every Woman Every Child movement have focused — correctly — on how to improve the care midwives give to women. But with this has come the emerging realization that in order for this to happen, we as a global health community must improve the care and attention we give to midwives.
It makes sense: ample evidence shows that if you educate, train, regulate, and support midwives better, you get better quality of care and rapid and sustained reductions in maternal and newborn mortality. Everyone wins! But how to achieve this is, as always, trickier. Last year, the World Health Organization released a report entitled Midwives’ Voices, Midwives’ Realities: Findings from a global consultation on providing quality midwifery care. This report was unique not only for its scale (it was the largest global survey of midwifery personnel to date) but also for the central questions it posed: what support and systems are needed to ensure that midwives can provide good-quality care, and what are the challenges in doing so?
The results were riveting, confirming that midwives have an in-depth awareness of critical factors to improve care. But those same results were also devastating, showing that midwives have almost no voice to share this awareness, press key issues toward dialogue, or implement creative solutions. Many of the same things that midwives need a voice to address are the things they say keep them silent: disrespect, subordination by the medical profession, gender discrimination, and lack of leadership and professional development opportunities.
Creating strong midwifery organizations is one of the most vital tactics to providing this voice. ACNM and its state-level affiliates, like mine in Washington, D.C., give the United States’ 12,000 or so certified nurse-midwives a respected voice in policy dialogue and are a tool for powerful legislative and social advocacy to advance clinical excellence and policies and regulations that support high-quality midwifery care. Most midwives in low- and middle-income countries don’t have access to anything like this, but they want it, badly: The midwives surveyed for the Midwives Voices, Midwives’ Realities report repeatedly cited the need for strong professional midwifery associations, from Yemen to Rwanda to Spain. The less of a voice the midwives reported having, the more they wanted midwifery associations to give them that voice. Professional associations represent a clear and viable way for midwives to share knowledge and solutions and fully participate in improving MNH in their countries, through improved recognition of the importance of midwives, communication with groups including the public and other health professionals, professional development opportunities, social support networks, networking, opportunities to develop leadership capabilities, and paths to leadership roles within the health system.
The International Confederation of Midwives set the theme of this year’s International Day of the Midwife as “Midwives, Mothers, and Families: Partners for Life” because “midwives everywhere understand that by working in partnership with women and their families they can support them to make better decisions about what they need to have a safe and fulfilling birth.” I — and every midwife I know — wholeheartedly support this idea. But in turn, the global health community must also be partners to midwives and support them by developing and enhancing professional midwifery associations. There are many paths to doing so, including technical assistance and financial support to improve the organization and leadership capacities of nascent midwifery associations, and supporting research that formally evaluates the links between strong midwifery associations and improved MNH outcomes. A little support can go a long way in making these associations powerful agents of change.