A Voice for Midwives is a Voice for Progress
May 3, 2019 | 2 Minute ReadA certified nurse-midwife, Emma Clark shares her thoughts on why midwives matter and why "investments in midwives are investments in our future."
Several years ago, a colleague was telling me about his efforts to introduce a new family planning method in one of the countries he worked in. “The women just weren’t interested in this method,” he said, frustrated. Initially, he and his team of experts couldn’t figure out why. They’d done a lot of legwork to plan the introduction. But a chance encounter with a midwife—the cadre that provided most of the reproductive, maternal, and newborn health care in that country—eventually told him about a cultural taboo, widespread but personal enough that most women wouldn’t feel comfortable discussing it. The midwives had the knowledge and experience to highlight the issue. Hadn’t they been consulted, I asked. He shrugged, looking bashful. “In hindsight, we definitely should have.”
This conversation spurred me—a midwife myself— to explore an array of family planning projects to see how often midwives were included in plans to introduce new family planning products. When I found minimal results, I gradually expanded my search to how often midwives were incorporated into general reproductive, maternal, newborn, and child health program planning overall. And still, very little.
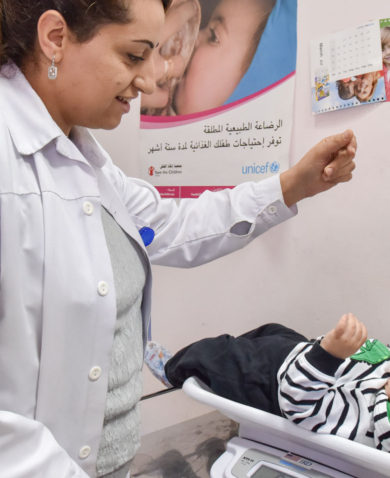
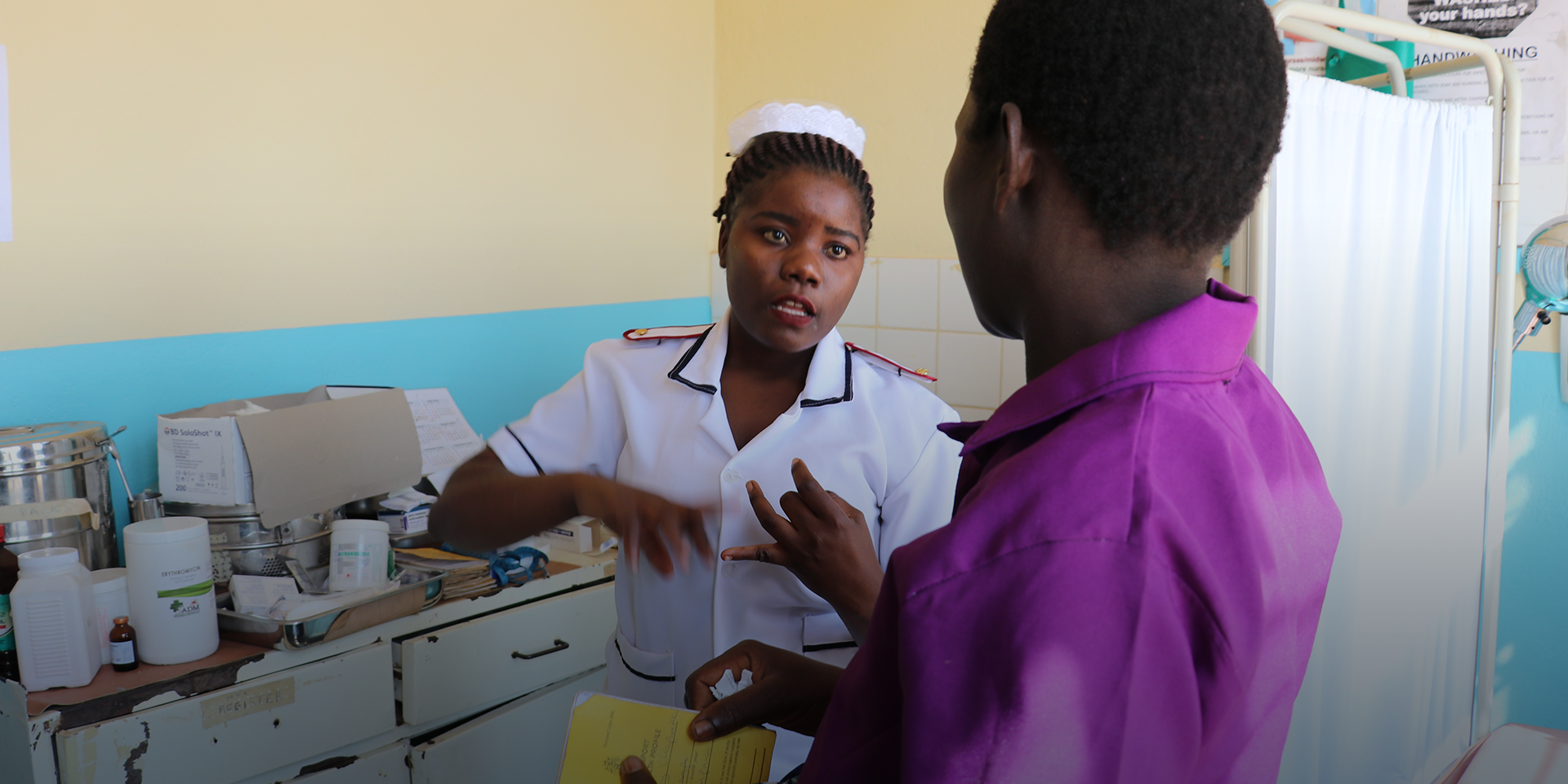
Midwives are on the front lines of providing essential reproductive, maternal, and newborn health services to a huge number of people globally. We’re privy to significant insights into our clients lives and the factors that shape the decisions that families make about how, when, and where they seek these health services. Because quality, access, and demand remain persistent challenges in meeting the ambitious Sustainable Development Goals, midwives should be sought after to provide perspective and insight into how to improve reproductive, maternal, and newborn outcomes.
And yet…they’re not. Even as many countries have translated increased global acknowledgement of the critical role of midwives into new approaches intended to improve the quality of midwifery services, they’ve consistently missed significant incorporation of perspective and feedback from midwives themselves. Midwives remain absent from leadership roles within ministries of health, as routine participants in formation of relevant policy, and in roles such as thought leaders, district supervisors, and participants in national and international maternal, newborn, and child health efforts. The landmark 2016 report “Midwives’ Voices, Midwives’ Realities” cataloged many of the underlying reasons why midwives are frequently excluded from the policy table, and why they struggle to have an audible voice in advocacy for themselves and the women they serve. But now, two years later, the report has lost its initial momentum, and little has changed. Midwives voices are still absent, or silenced, or yelling into an empty room. The result is missed opportunities to get insight into what women and their families need, maximize what midwives can offer, and provide what midwives need to succeed in their challenging roles.